Deep Vein Thrombosis (DVT)
When blood moves too slowly in your veins, it can cause blood cells to clump and cluster (a blood clot or thrombus).
Deep vein thrombosis (DVT) is a condition in which a blood clot forms in the a vein located within the deep venous system in the leg, thigh, or pelvis. Veins in the deep venous system lay underneath muscle tissue and are no visible to the naked eye.
Your health is our priority.
Contact us today.
How do Blood Clots Form?
The venous system in the legs consists of two sub systems – the superficial venous system and the deep venous system. Deep veins are, as the name suggests, located deep within the body and lay under muscle tissue and are not visible to the naked eye. On the other hand, superficial veins are located just below the skin and are easily visible. Typically, blood flows from the superficial veins into the deep venous system through perforator veins.
Both the perforator and superficial veins have valves that allow blood to
flow in one direction – back to the heart.
When blood travels too slowly or pools in the veins, platelets can stick together. While a blood clot (thrombus) in the deep venous system of your leg is not dangerous by itself, it can become life-threatening when it breaks and travels up towards the pulmonary vein. When a blood clot blocks a pulmonary artery, it decreases the amount of oxygen absorbed in the blood. This can cause a life-threatening condition known as pulmonary embolism.
Deep vein thrombosis (DVT) is considered a medical emergency.
Studies show that 10-30% of individuals who develop DVTs in the legs experience life-threatening complications within a month of diagnosis.
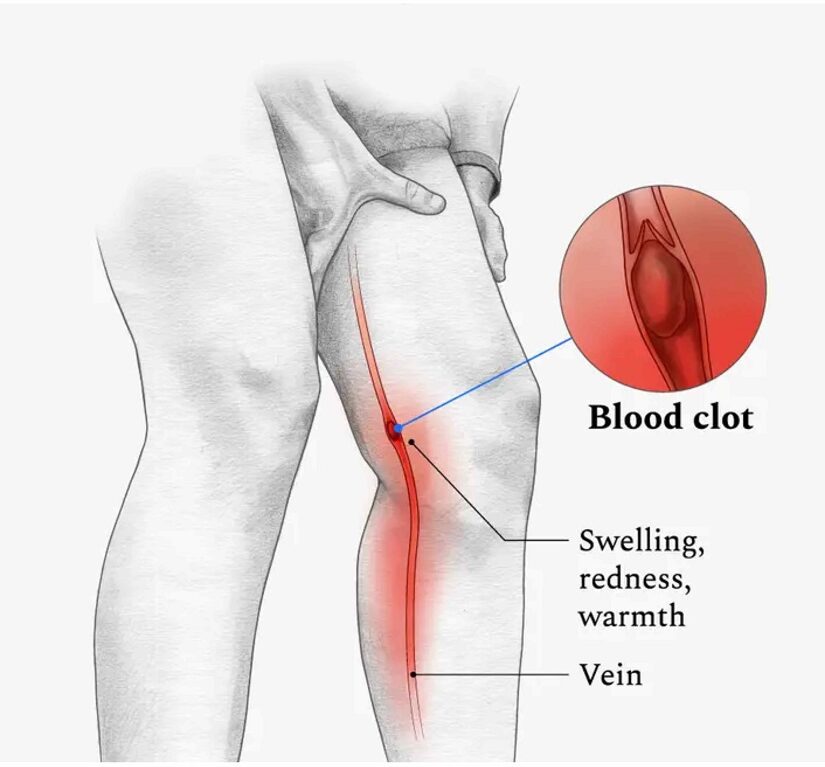
Deep Vein Thrombosis – Symptoms
Like other disorders that affect the venous system, some individuals with DVT may not notice any symptoms.
However, if symptoms do develop, people with deep vein thrombosis (DVT) may experience the following:
- Sharp pain in the affected limb that starts in the calf
- Red or discolored skin on the affected limb
- Swelling in the affected limb
- Enlarged veins
- Concentrated warmth in the affected region
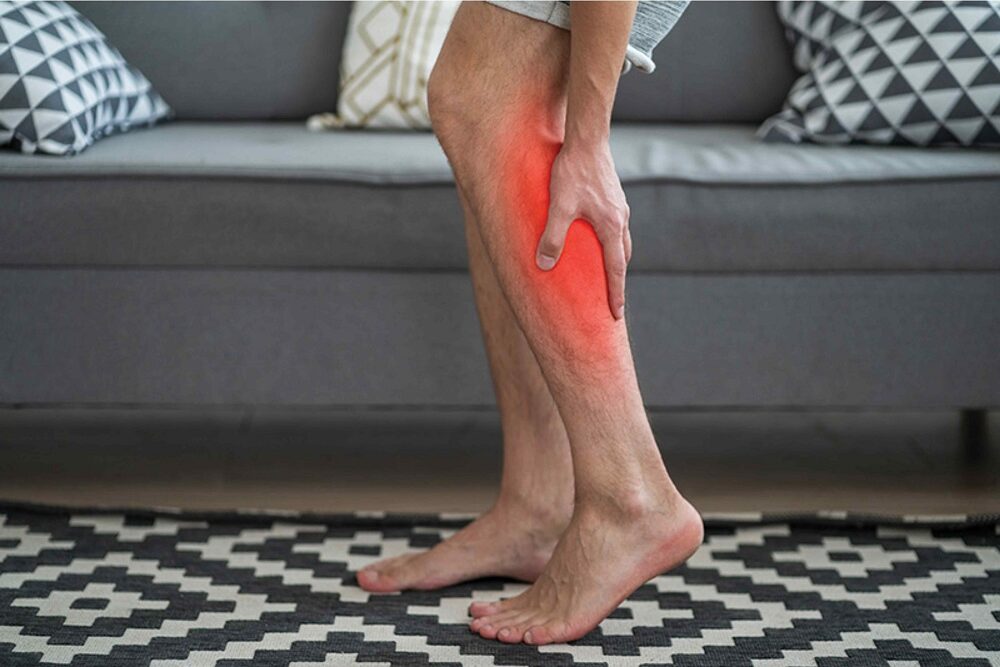
Deep vein thrombosis (DVT) usually affects only one of the legs. However, on rare occasions, the condition may develop in both legs.
If the blood clot (thrombus) breaks and travels up to the lung, a person suffering from pulmonary embolism may have the following symptoms:
- Sudden breathlessness or slow breathing
- Rapid breath
- Increased heart rate
- Chest pain that worsens when breathing deeply
Causes and Risk Factors of DVT
Sometimes, deep vein thrombosis (DVT) develops without a clear cause. Research has found, however, that DVT occurs due to
one or a combination of the following underlying conditions and risk factors:
Staying seated for an extended period creates a lack of movement in the muscles in your lower legs, making it hard for blood to circulate.
Surgery or an injury can damage the veins, leading to slow blood flow and ultimately increasing the risk of a blood clot. The use of general anesthetics also tends to widen the veins, increasing the likelihood of blood pooling.
Individuals who may have inherited disorders such as Factor V Leiden thrombophilia that cause blood clots are also at high risk of contracting deep vein thrombosis (DVT).
During pregnancy, the pressure exerted on veins in the leg and pelvis increases. Studies show that women have an increased likelihood of contracting deep vein thrombosis (DVT) during pregnancy until about six months after delivery.
Late-stage colon, breast, and pancreatic cancers also lead to a higher risk of deep vein thrombosis (DVT). Additionally, cancer treatments such as chemotherapy, surgeries, and central venous catheters increase the risk of contracting DVT.
Conditions that impact the heart’s ability to pump blood throughout the body can lead to clots and bleeding. For instance, congestive heart failure and heart attack can increase the risk of developing deep vein thrombosis (DVT) as they affect the way in which blood is pumped throughout the body.
Excess weight and obesity put pressure on the blood vessels, especially those in the legs and pelvis. As such, these individuals have increased risks of contracting deep vein thrombosis (DVT).
The nicotine that is found in cigarettes increases your blood platelets and makes them sticky. As a result, they are more likely to clump together and create a dangerous blood clot.
Varicose veins are another condition that can lead to DVT. Varicose veins cause blood to pool in the veins, increasing the chance of blood clot formation.
While DVT can affect both men and women at any age, individuals over the age of 40 are at an increased risk.
Birth control pills and hormone replacement therapy have estrogen hormones that increases the likelihood of a blood clot.
When you have an infection, your blood is more likely to clot. This can lead to DVT. Inflammation is also a significant contributor to DVT because your risk of DVT increases with the level of inflammation present in your body.
Diagnosing Deep Vein Thrombosis (DVT)
Deep vein thrombosis leads to various health problems, including life-threatening conditions such as pulmonary embolism.
If you suspect that you have symptoms that are conducive with deep vein thrombosis, seeking treatment immediately is crucial. Your physician will ask you various questions about your medical history and symptoms before performing a physical examination. They can also run diagnostic tests that help to determine if you have DVT or not.
There are two types of diagnostic tests:
Ultrasound
Venogram
An ultrasound test is effective in detecting blood clots.
The doctor uses a handheld device that sends sound waves into the blood vessels. The picture is then displayed on a computer
that shows the condition of your veins and whether or not
there is a clot present.
To get an even clearer picture, the doctor may request a venogram. During a venogram, a special dye is injected into your veins and projected onto an X-ray imaging scan. The movement of the dye is then capture on the X-ray and is used to identify areas of your veins that may be clotted.
Complications of DVTs
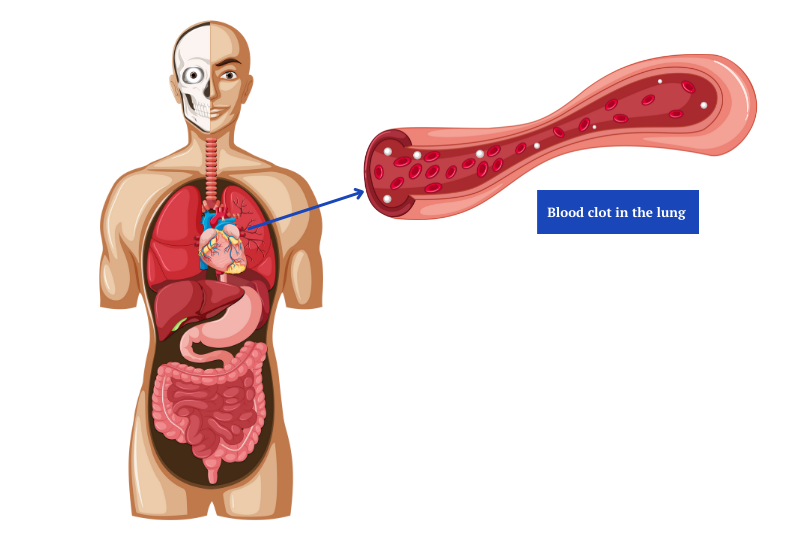
Pulmonary Embolism (PE)
PE is a severe DVT complication that develops if a blood clot travels through the blood vessels and reaches the lungs. When the blood clot is stuck, it disrupts the flow of blood into the lungs. A medium-sized clot can lead to intense chest pain and breathing problems. In more severe cases, the lungs can collapse and even lead to heart failure.
Post-Thrombotic Syndrome
People with recurrent DVT are at high risk of post-thrombotic syndrome.
You may experience the following symptoms if you have this condition:
- Heavy legs
- Calf swelling
- Tired legs
- A pulling sensation in the affected limb
- Varicose veins
- Skin discoloration/redness on the affected limb
- Fluid buildup in the affected limb
- Skin thickening or ulcers on the affected limb
Why Monterey Bay Vascular?
At Monterey Bay Vascular, we offer coordinated care to prevent, diagnose, and treat vascular disease.
We understand, everyone deserves to live a long, happy life. Vascular disease may lead to limb loss and other life-threatening conditions such as pulmonary embolism. Our licensed vascular surgeon uses state-of-the-art tools and technology to tackle all problems related to your vascular system. Thanks to our vast wealth of experience, we also work with our patients to develop a unique solution that fits your needs. Contact us today to learn more about the vascular treatments we offer and schedule an appointment today!