Varicose veins are enlarged, bulging veins that run just beneath the surface of your skin.
These problematic veins often appear on the legs and feet. They develop when the valve in the veins stops working properly. When veins begin to malfunction, blood can flow backwards and start to “pool.” These veins are usually harmless. However, in some cases, they can cause pain and discomfort.
Deep varicose veins are not visible but tend to cause aching or swelling throughout the affected limb. Sometimes, blood clots can develop. When inflamed, these veins become tender to touch. They also impede blood flow – causing itchy skin, aching, and swollen ankles in the affected limb. In severe cases, the varicose vein may rupture, leading to varicose ulcers on the skin.
Symptoms of Varicose Veins
- A heavy or achy feeling in your feet
- Throbbing, burning, muscle cramping in your lower legs
- Itching on your lower legs
- Worsening pain, especially after standing or sitting for an extended period
- Skin discoloration on the affected limb
- Swelling in the legs
- Leg cramps at rest, especially at night
Varicose Vein FAQs
Varicose veins affect about 23% of all americans.
Varicose veins are relatively common, especially if you have a family history of the condition. The disorder affects men and women of any age but most frequently affects women in their childbearing years and the elderly.
- Varicose veins occur when the valve inside the veins fails to function properly. Healthy veins allow blood to flow efficiently back to the heart. Backward blood flow is prevented by small valves that open and close. In some instances, damaged or weakened veins cause blood to flow backward. The blood collects in the vein, causing it to be swollen/enlarged.
In other scenarios, weakened or damaged veins can also cause blood to pool. When the veins become weak, they are unable to push blood back to the heart. This causes the blood volume in the vessels to increase, leading to varicose veins. Some of the other less common causes are listed below.
- Inflammation of the veins (phlebitis)
- Congenital abnormalities of the veins
- Blood clots and other conditions that may obstruct the flow of blood in the veins
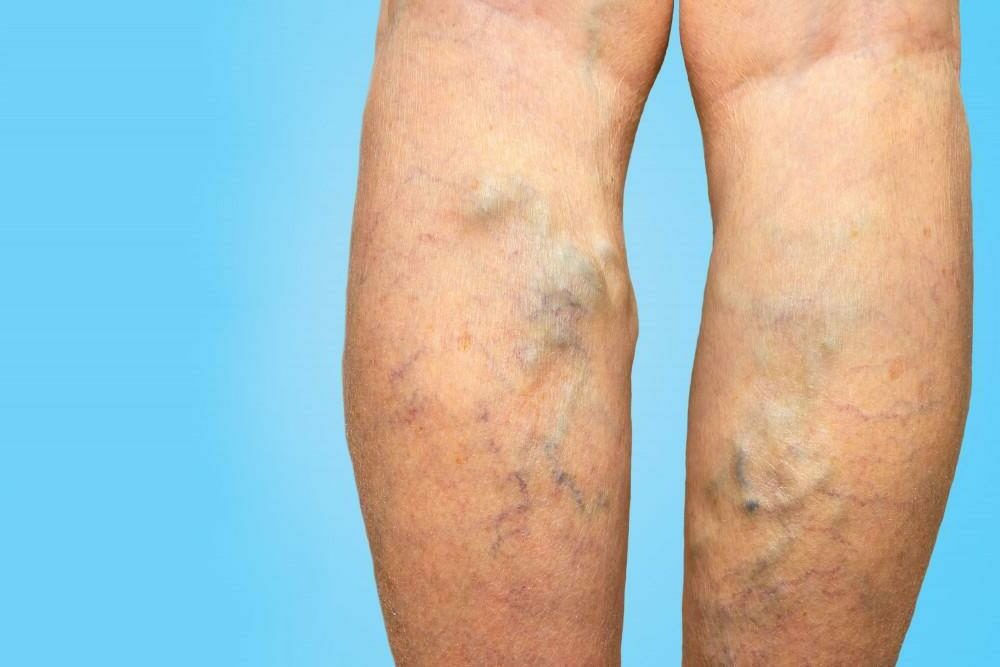
Complications of Varicose Veins
Non-Healing Ulcers or Wounds
Sometimes, varicose veins lead to painful ulcers that form on the skin near the affected veins and ankles. Before forming the ulcer, you will note a discolored spot that deteriorates to become a painful non-healing ulcer. In case you suspect the formation of an ulcer, seek medical intervention immediately.
Blood Clots
Chronic inflammation in your legs requires medical attention as it most often indicates a blood clot. Blood clots (thrombus) are dangerous as they can travel up the veins, and into the lungs and brain causing a pulmonary embolism or stroke. When blood pools in the veins, the affected area becomes painful, swollen and often is warm to the touch.
Bleeding
When the pressure builds up in the veins close to the skin, they eventually burst, causing minor bleeding. While the skin breakout may be minor, seeking medical attention is crucial to prevent further complications.
Causes of Varicose Veins
Varicose vein risk increases with age. As we age, the valves in our veins become weak. The wear and tear will eventually allow the blood to leak back into the vein where it collects instead of flowing upwards to the heart. When the blood pools the veins begin to twist and enlarge.
Being overweight exerts extra pressure on the veins, making it hard for them to push the blood to your heart.
Studies show that women are more susceptible to varicose veins than men are. Hormonal changes during pregnancy or before menstruation cause the venous walls to relax, leading to blood flowing backwards. Hormone treatment such as birth control pills can also increase your likelihood of developing the condition.
The hormonal changes that occur during pregnancy can also increase your risk for varicose veins. When you become pregnant, the blood volume in the body increases to help support the growing fetus. Unfortunately, the increased blood might be too much for your veins to push back to the heart from your feet, resulting in enlarged veins.
Research also shows that individuals with a family history of varicose veins have an increased chance of developing the condition.
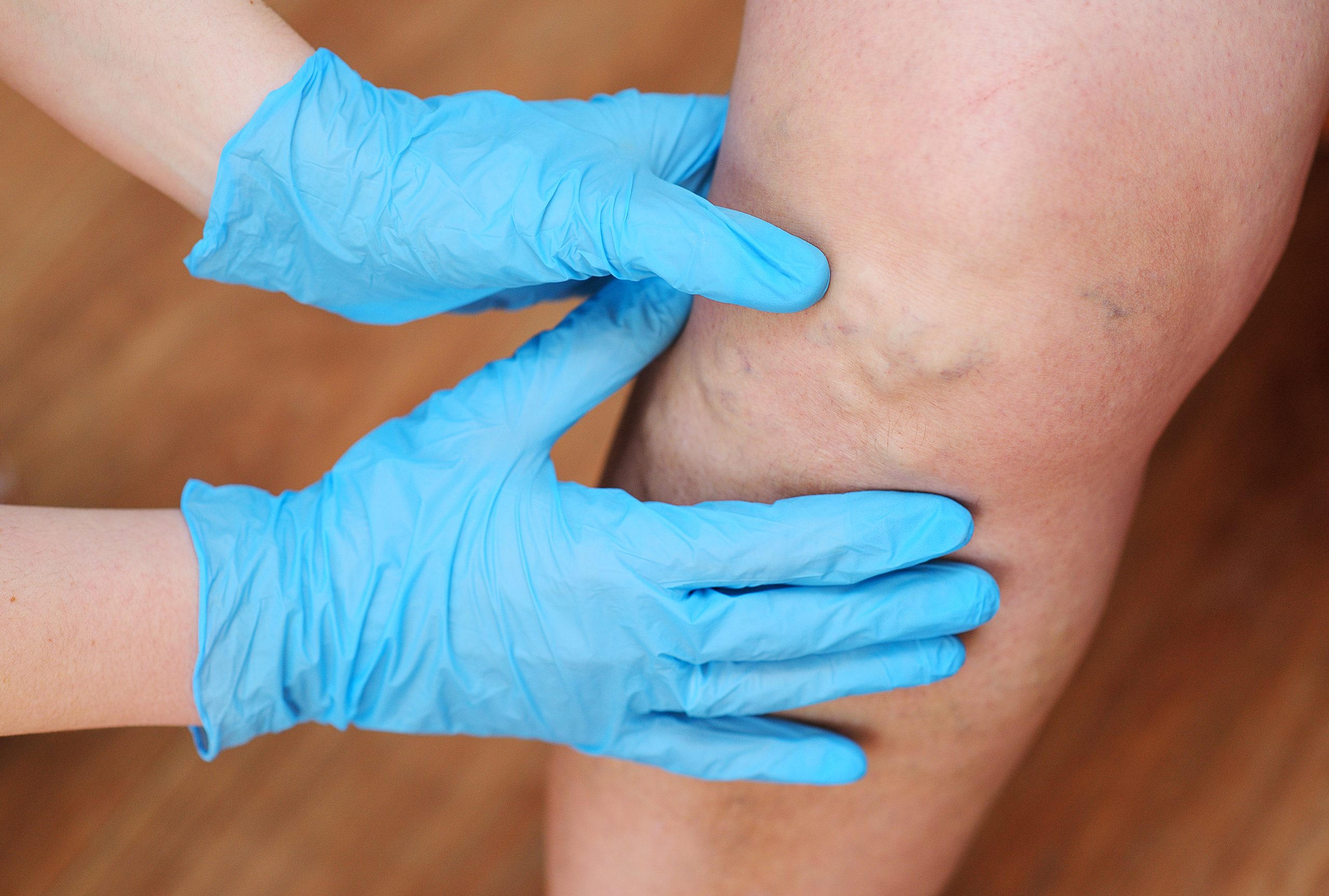
Treatment & Prevention
Treatment for varicose veins may include self-care measures, compression stockings, and non-surgical procedures. Minimally invasive procedures are often performed in an outpatient center, which means you usually go home on the same day.
- Regular Exercise
- Moving Around Regularly
- Elevating your Feet
- Maintaining Healthy Weight
- Avoid Wearing Tight-Fitting Clothes
- Supportive Pantyhose & Compression Socks
Compression therapy is the most conservative treatment option. Compression stockings are designed to apply specific pressure to the legs to alleviate discomfort and swelling. They can be purchased at your local pharmacy or at your vascular specialist office.
Reach Out to Our Team
At Monterey Bay Vascular, we offer coordinated care to prevent, diagnose, and treat vascular disease.
We understand, everyone deserves to live a long, happy life. Vascular disease may lead to limb loss and other life-threatening conditions such as pulmonary embolism. Our licensed vascular surgeon uses state-of-the-art tools and technology to tackle all problems related to your vascular system. Thanks to our vast wealth of experience, we also work with our patients to develop a unique solution that fits your needs. Contact us today to learn more about the vascular treatments we offer and schedule an appointment today!