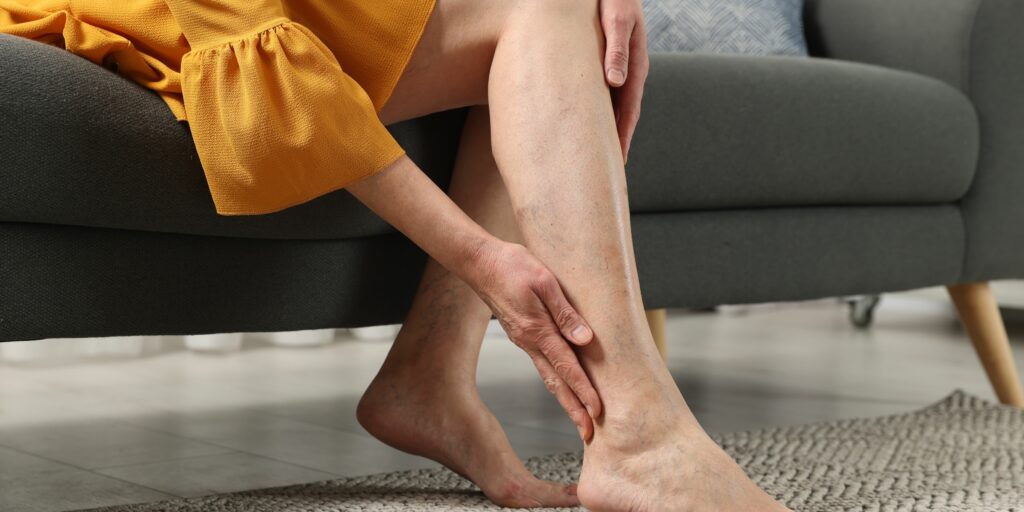
Varicose veins are enlarged, twisted, and swollen in the legs and feet, causing discomfort and pain for millions worldwide. Understanding and managing their causes is vital for maintaining vascular health and overall well-being.
How do varicose veins develop?
Varicose develops when valves weaken, causing inefficient blood flow and enlargement, especially in the legs and feet, due to increased pressure. Factors include weakened valves, inefficient flow, and pressure. Promptly addressing venous insufficiency prevents complications like chronic venous disease. Lifestyle choices, exercise, and treatments, including surgery, help manage vein health.
Anatomy of Healthy Veins
To better understand varicose veins, it is essential to recognize the differences between healthy veins and varicose veins. Healthy veins have smooth and elastic walls, allowing blood to flow efficiently towards the heart. In contrast, varicose veins have weakened walls and faulty valves, causing blood to pool and veins to become enlarged and twisted.
Common Locations
Varicose veins can occur in various parts of the legs and feet, with certain areas being more prone to their development. The most common locations include the back of the calves, inside of the legs, and around the ankles. Understanding the locations of varicose veins can help individuals identify potential issues and seek appropriate medical attention.
Primary Causes
Genetic Predisposition
Genetics plays a significant role in the development of varicose veins. If one or both parents have a history of varicose veins, the risk of developing the condition is higher. While genes may not be entirely responsible for varicose veins, they can make individuals more susceptible to the condition
Age-related Factors
As people age, the risk of developing varicose veins increases due to natural wear and tear on the veins’ valves. Over time, the valves may weaken, causing blood to pool in the veins and leading to the development of varicose veins.
Gender and Hormonal Influence
Women are more likely to experience varicose veins than men. Hormonal changes during puberty, pregnancy, and menopause can affect vein elasticity and increase the risk of developing varicose veins.
Secondary Causes
Prolonged Standing or Sitting
Occupations that involve extended periods of standing or sitting can contribute to the development of varicose veins. This is because staying in one position for too long can impede blood circulation, leading to vein enlargement.
Obesity and Weight-related Factors
Excess body weight puts additional pressure on the veins, making overweight individuals more prone to varicose veins. Weight management and maintaining a healthy lifestyle can help reduce the risk of developing the condition.
Pregnancy and Hormonal Changes
Pregnancy causes hormonal shifts and increased blood volume, leading to varicose veins in some women. These veins may improve after childbirth, but the risk of developing varicose veins may persist in future pregnancies.
Symptoms
Visible Appearance
One of the most apparent signs of varicose veins is the visibility of enlarged twisted veins beneath the skin’s surface. These veins may appear bluish or purplish in color and can be easily seen on the legs and feet.
Pain, Discomfort, and Heaviness
Varicose veins can cause aching pain and discomfort, especially after prolonged periods of standing or sitting. Individuals with varicose veins may experience a heavy sensation in their legs, which can affect their daily activities.
Itching and Skin Discoloration
The affected area may itch, and the skin around the varicose veins may become discolored. Itching can be bothersome and may lead to scratching, which can further irritate the skin.
Swelling and Edema
Swelling, particularly in the ankles and feet, is a common symptom of varicose veins. The accumulation of fluid in the affected area can lead to edema, which can worsen as the day progresses.
What Worsens Varicose Veins?
Lifestyle Factors and Impact
Sedentary Lifestyle
A sedentary lifestyle, characterized by prolonged periods of inactivity, can contribute to poor blood circulation, exacerbating varicose veins. Incorporating regular physical activity into daily routines can improve blood flow and help manage varicose veins.
Lack of Exercise
Regular exercise is beneficial for cardiovascular health and can help prevent varicose veins from worsening. Activities such as walking, swimming, and cycling can promote blood circulation and reduce the risk of vein enlargement.
Diet and Its Role
A balanced diet rich in fiber, antioxidants, and essential nutrients plays a role in maintaining vascular health and preventing varicose veins. It is essential to avoid excessive salt intake, as it can contribute to water retention and worsen swelling.
Age and Other Factors
Age-related Risk Factors
As mentioned earlier, age is a significant risk factor for developing varicose veins. The natural aging process leads to wear and tear on the veins, causing them to weaken and lose their elasticity.
Varicose Veins in Younger Individuals
While varicose veins are more common in older adults, they can also occur in younger individuals. Certain genetic factors, lifestyle choices, and occupations can increase the risk of developing varicose veins at a younger age.
Impact of Aging on Existing Varicose Veins
Varicose veins may worsen over time, especially if left untreated or not managed properly. As individuals age, it becomes essential to prioritize the management and treatment of varicose veins to prevent further complications.
The Two Main Causes of Varicose Veins
Understanding Primary and Secondary Causes
Distinguishing between primary and secondary causes helps in understanding the condition’s root factors. Primary causes are often inherent, while secondary causes are influenced by lifestyle and environmental factors.
How They Interact and Contribute
Both primary and secondary causes can work together to exacerbate varicose veins. For example, a person with a genetic predisposition to varicose veins may experience worsening symptoms if they have a sedentary lifestyle or are overweight.
The Leading Cause
Identifying the Primary Culprit
Determining the main cause of varicose veins can aid in targeted treatment. While primary causes are often beyond an individual’s control, addressing secondary causes can help manage the condition effectively.
Prevalence and Impact
Understanding the prevalence and impact of the leading cause is crucial for addressing the condition effectively. This knowledge can inform public health initiatives and preventive measures.
What Causes Varicose Veins to Worsen?
Progression of Varicose Veins
Varicose veins can worsen over time if left untreated or not managed properly. As the condition progresses, individuals may experience increased discomfort and cosmetic concerns.
Aggravating Factors
Certain factors can accelerate the progression of varicose veins, making them more uncomfortable. These factors may include a sedentary lifestyle, obesity, and hormonal changes.
Preventive Measures
Taking proactive measures can help prevent varicose veins from worsening. Lifestyle changes such as regular exercise, weight management, and elevating the legs can promote better circulation.
Varicose Veins and Blood Clots
Understanding the Connection
There is a relationship between varicose veins and the risk of developing blood clots. Blood clots may form in the enlarged varicose veins, leading to potential complications.
Assessing the Risk
Identifying risk factors and assessing individual risk can guide preventive actions. Individuals with a history of blood clots or those with other risk factors may require closer monitoring.
Preventive Strategies
Managing varicose veins effectively can reduce the risk of associated blood clots. Compression stockings, regular exercise, and proper hydration can be effective preventive measures.
Red Flags of Varicose Veins
Recognizing Serious Symptoms
Knowing when varicose veins may indicate a more severe underlying condition is essential. If individuals experience sudden, severe pain or swelling, or they notice wounds that are not healing quickly, they should seek immediate medical attention.
When to Seek Medical Attention
Promptly seeking medical advice is essential for identifying and addressing potential complications. Individuals should not ignore persistent symptoms or sudden changes in their varicose veins.
Varicose Veins’ Impact on Cardiovascular Health
Association with Heart Health
While varicose veins are not typically considered a serious cardiovascular condition, they can affect blood flow and circulation.
Addressing Concerns and Misconceptions
Dispelling myths and addressing concerns about varicose veins and heart health can help individuals make informed decisions about their vascular health.
Do Clogged Arteries Cause Varicose Veins?
Understanding Arterial and Venous Systems
Distinguishing between arterial and venous issues is essential to clarify the relationship between clogged arteries and varicose veins. Arteries carry oxygen-rich blood away from the heart, while veins return oxygen-depleted blood to the heart.
Clarifying the Relationship
Contrary to popular belief, clogged arteries do not cause varicose veins. Clogged arteries involve atherosclerosis, where plaque builds up inside the arteries, while varicose veins result from weakened valves in the veins.
Taking Charge of Your Veins
Key Points Discussed
Emphasizing the role of genetics, age, lifestyle factors, and preventive measures can empower individuals to take control of their vascular health.
Empowering Yourself with Knowledge
Knowledge is essential for informed decisions regarding treatment and prevention. Understanding the causes and symptoms of varicose veins empowers individuals to take charge of their vascular health. For more resources and information, feel free to visit our website or visit our office at 945 Blanco Circle Suite A, Salinas, CA 93901, and 3275 Aptos Rancho Road Suite A & B, Aptos, CA 95003.
Conclusion
Varicose veins are a prevalent vascular condition that affects a significant portion of the population. Understanding the causes and symptoms of varicose veins is essential for timely medical intervention and preventive measures. If you experience varicose veins or related symptoms, seeking professional advice is crucial for proper management. Emphasizing self-care and making informed decisions can empower individuals to take charge of their vascular health.